
Plastic Surgery for Disabled People: Helpful Things to Know
From Access to Surgery - What Actually Matters
Plastic surgery for disabled people includes choosing access to suitable facilities, clear communication with clinicians, and recovery planning that reflects real-world barriers. With the right support, surgery can improve comfort, function, or confidence — but access remains uneven, and the system you are working your way through depends heavily on where you live.
Key insights and access realities
| Key Insight | Why It Matters |
|---|---|
| Disabled people seek both functional and cosmetic procedures | Decisions are personal and varied, not limited to medical necessity |
| Access barriers still exist in many clinics | Inaccessible equipment or spaces can affect safety and dignity |
| Legal protections exist in both the UK and US | But enforcement is inconsistent and requires disabled people to push back |
| Preparation needs to be more detailed | Planning reduces risk and helps healthcare teams understand real needs |
| Recovery often requires adapted support | Standard advice may not reflect mobility, energy, or care needs |
| Peer experiences offer practical insight | Disabled people often learn more from each other than from leaflets |
What is plastic surgery for disabled people?
Plastic surgery for disabled people refers to cosmetic or reconstructive procedures carried out with adjustments for access, safety, and individual needs. This can include changes to equipment, longer planning timelines, and tailored recovery support.
The difference is rarely the procedure itself. It is the environment around it — whether clinics are accessible, whether staff understand disability, and whether care plans reflect real life rather than a standard patient template.
For readers in the US, providers such as the New Jersey Breast Reduction Center highlight how adapting surgery around mobility, pressure care, and recovery support can improve outcomes for patients with different access needs.
Why disabled people choose plastic surgery
Function, comfort, and confidence all play a role
Some disabled people pursue surgery to reduce pain or improve movement. Breast reduction, for example, can ease back strain for wheelchair users. Scar revision may reduce friction or improve range of motion. Reconstructive surgery after injury or pressure sores can restore both function and appearance.
Others choose cosmetic procedures for the same reasons as anyone else. Feeling comfortable in your appearance matters. That includes disabled people, even though this is often questioned more than it should be.
Lived experience: Ferve’s perspective
Ferve is a paraplegic woman who works as a patient coordinator at a plastic surgery clinic. She chose procedures including lip fillers and buccal fat removal — not for medical reasons, but for her own confidence.
“Having these minor changes in your body does not make you 100% fake! If this will make you happy, go for it,” Ferve explains. “Getting fillers really helped boosting my confidence and now I am a lot more relaxed while taking photos.”
Her story reflects a wider reality — disabled people are not limited to medical justifications when making choices about their bodies, and shouldn’t have to be. Read Ferve’s full story here.
The Timeline of Preparing for Surgery
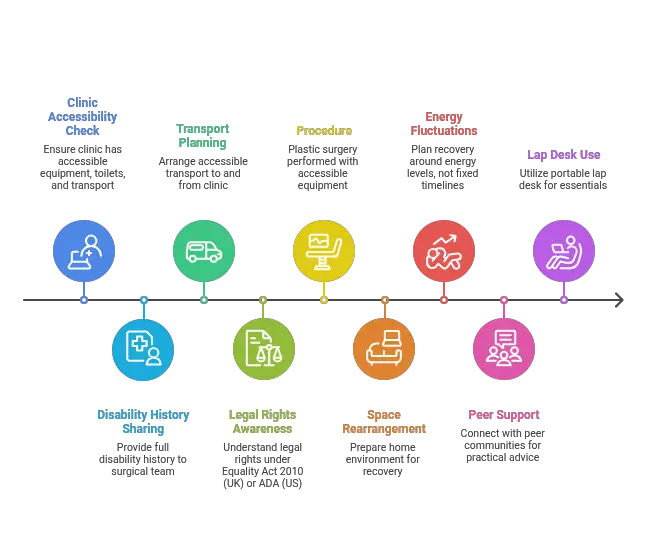
Common procedures and how they relate to daily life
Procedures linked to function
- Breast reduction to reduce strain during wheelchair use
- Scar revision to improve movement or reduce irritation
- Reconstructive surgery after injury or pressure sores
- Correction of congenital differences such as cleft palate or limb variations
Procedures linked to appearance
- Facial procedures such as fillers or contouring
- Body contouring after weight changes linked to disability
- Gender-affirming surgeries with mobility considerations
In practice, the line between function and appearance is often blurred. A procedure might improve both comfort and confidence at the same time — and both are valid reasons to pursue surgery.
Access barriers in plastic surgery settings
Where systems still fall short
Access is one of the biggest practical issues. A survey published in Plastic Surgery Practice found that only 54.5% of plastic surgery practices confirmed they were ADA-compliant, with 27.3% admitting non-compliance and 18.2% unsure of their status.
When basic accessible equipment is missing — adjustable examination tables, wheelchair scales, safe transfer support — the impact is not minor. It affects dignity, safety, and whether someone can go ahead with surgery at all.
What good access looks like in practice
The best facilities — whether NHS units in the UK or private clinics in the US — treat accessibility as standard rather than an add-on. That means accessible entrances, wide doorways, height-adjustable beds, hoists where needed, and staff who ask the right questions rather than waiting to be told.
It is worth checking these details before booking, not on the day of surgery.
Legal rights: UK and US compared
In the UK: the Equality Act 2010
In the UK, the Equality Act 2010 requires healthcare providers to make reasonable adjustments for disabled patients. This covers both NHS and private providers. Reasonable adjustments can include accessible appointment times, physical adaptations, and communication support.
In practice, “reasonable” is interpreted broadly and complaints can be taken to the Care Quality Commission or NHS England. Private providers can also be challenged through the Equality and Human Rights Commission.
In the US: the ADA and Section 504
In the US, the Americans with Disabilities Act requires clinics and hospitals to provide reasonable accommodations — accessible examination tables, sign language interpreters, wheelchair-accessible spaces. Section 504 of the Rehabilitation Act applies to any provider receiving federal funding.
Enforcement has teeth. In cases brought against major US health systems, settlements have required facilities to install accessible examination tables, wheelchair scales, and deliver disability awareness training across entire organisations. These are not theoretical protections — disabled patients have used them successfully.
What this means in practice, wherever you are
Whether you are in Manchester or New Jersey, you have legal grounds to ask for what you need. The difference is in how easy it is to enforce. Knowing your rights before you walk through the door changes the conversation.
NHS vs private: what the difference means for disabled patients
In the UK, reconstructive and functional plastic surgery — such as scar revision, post-injury repair, or breast reduction causing significant physical problems — is often available on the NHS. Purely cosmetic procedures generally are not, though NHS trusts do have an exceptional treatment panel process for cases that fall into a grey area. The NHS sets out what may be funded and when.
For disabled people, this distinction can make a real difference in practice. A functional procedure — breast reduction for a wheelchair user with documented back pain, for example — may meet NHS criteria where the same procedure for a non-disabled person would not. Some disabled people report needing to clearly explain how a procedure affects daily function — such as pushing a wheelchair or managing pain — before it is taken seriously in referral decisions. It is worth making this case explicitly with your GP or referrer, particularly if your disability changes how the condition affects your daily life, rather than assuming a procedure falls outside NHS scope.
If you are going privately, the same legal obligations apply. Private providers must still meet Equality Act requirements, make reasonable adjustments, and not refuse or disadvantage disabled patients. The NHS has also introduced a Reasonable Adjustments Digital Flag — a system allowing disability and adjustment needs to be recorded and shared across care settings, reducing the need to repeat yourself at every appointment. Ask your GP practice whether this has been set up on your record.
Preparing for surgery: what actually helps
Planning beyond standard checklists
- Discuss mobility, transfers, and positioning in detail with the surgical team
- Check whether the facility’s equipment actually meets your needs — not just on paper
- Plan accessible transport for surgery day and all follow-up appointments
- Arrange support from someone who knows your routine, not just a general carer
- Share a full medication list including anything related to your disability
It is worth writing all of this down. Not because you should have to, but because it reduces the risk of being misunderstood in a system that often assumes standard bodies and routines.
Practical tools that make recovery easier
Some disabled people adapt their recovery setup using practical tools that rarely appear in clinical discharge notes. Creating a stable surface for meals, medication, or devices can make a significant difference when you are limited in what you can reach or carry.
Some wheelchair users describe setting up their recovery space with tools like portable lap desks for wheelchair users (Disability Horizons Shop) to keep medication, food, and devices within reach when movement is limited.
Managing risks specific to disability
Pressure care and positioning
For people with reduced sensation or mobility, pressure management during and after surgery is critical. Clinical guidance recommends regular repositioning — every two hours when lying down, more frequently when seated — and the use of pressure-relieving surfaces throughout the hospital stay and recovery period.
Circulation and clot prevention
Wheelchair users and people with limited mobility may face higher risks of deep vein thrombosis after surgery. This can be managed with planned movement schedules, compression garments, and anticoagulant medication where clinically appropriate. Raise this specifically with your surgical team before the procedure.
Why this matters
These risks are not reasons to avoid surgery. They are reasons for better planning and for choosing clinicians who understand disability rather than those who treat it as a complication to work around.
Recovery: what disabled people say actually works
Peer insight from disabled communities
Online communities share practical advice that rarely appears in official discharge guidance. Wheelchair users discuss temporarily switching to powered mobility during recovery to protect healing tissue. Others describe adjusting daily routines entirely for several weeks to avoid strain on surgical sites.
People who have had breast reduction surgery describe a difficult recovery that led to significant long-term improvement in comfort and mobility — particularly for those whose disability already placed strain on their upper body. That honesty about short-term difficulty versus long-term benefit is often missing from clinical summaries.
Adapting your environment
- Rearrange your space before surgery to reduce unnecessary transfers during recovery
- Arrange wound care support if reach or dexterity is limited
- Plan for energy fluctuations rather than fixed recovery timelines
- Identify backup support in case your primary helper is unavailable
Psychological and social factors
Decisions about plastic surgery can carry extra weight for disabled people. There may be external opinions about what counts as “necessary” or assumptions that disabled people should be focused on other things. Neither of those is your problem to manage.
Support from peers, counsellors, or others with similar experiences can help ground decisions in your own priorities. Connecting with disabled people who have been through similar procedures — whether through online communities or disability organisations — often provides more practical reassurance than clinical consultations alone.
Making informed decisions
It often comes down to how you are treated in that first consultation. Ask questions, expect clear answers, and pay attention to whether the provider listens. A good provider adapts, respects your knowledge of your own body, and does not make you fight to be understood.
If that is missing — if you feel dismissed, rushed, or that your disability is being treated as an obstacle — it is reasonable to look elsewhere. Providers who work well with disabled patients exist, and they are worth finding.
Before you go: things worth checking
- Does the clinic have adjustable examination tables and accessible toilets?
- Have you shared your full disability history including medications and equipment needs?
- Is there someone who can advocate for you at appointments?
- Have you planned accessible transport for surgery day and follow-ups?
- Does your recovery space work for your mobility aids?
- Do you know your legal rights under the Equality Act (UK) or ADA (US)?
If you have been through plastic surgery as a disabled person and have advice to share, we would genuinely like to hear it. Email us at shop@disabilityhorizons.com