
8 myths about living with urinary catheters busted
This is an updated post from our archives. Living with a urinary catheter is often misunderstood, leading to various myths and misconceptions. This article debunks eight common myths about urinary catheters, providing accurate information to help readers better understand their use and management.
Catheters help folks empty their bladders and are a common sight in hospitals, especially when someone’s having surgery or is unconscious. But did you know that there’s a larger group who need catheters beyond just hospital patients? Loads of people with disabilities or health conditions rely on them because of injuries, illnesses, or impairments.
Our writer, Emma Purcell – who had a catheter fitted in 2018 – debunks 8 myths about living with catheters.
A urinary catheter is a flexible tube used to empty the bladder and collect urine in a drainage bag. They are usually inserted by a doctor or nurse.
They can either be inserted through the tube that carries urine out of the bladder (urethral catheter) or through a small opening made in your lower tummy (suprapubic catheter).
There are two main types of urinary catheters:
- Intermittent catheters – these are temporarily inserted into the bladder and removed once the bladder is empty.
- Indwelling catheters – these remain in place for many days or weeks and are held in position by an inflated balloon in the bladder.
I have cerebral palsy and was fitted with an indwelling suprapubic catheter in June 2018 because I was finding it difficult and laborious to access public toilets and frequently go to the toilet at home.
Other common uses for catheters include a weakened bladder, urinary retention, paralysis, spinal injury, multiple sclerosis (MS), Parkinson’s, pelvic organ prolapse, and many more.
Here are 8 myths society believes are true about living with urinary catheters…
1. Catheters are painful
Not at all. If anything, you hardly ever notice it. The only time I get some discomfort is if the tube is kinked causing a blockage, as this means I start to feel my bladder becoming full and not emptying properly.
The removal and insertion of catheters are definitely not pleasant. I have my catheter changed every six weeks by the district nurses. Other catheter users may get it changed every eight, 10 or 12 weeks, but I found the longer it stays in, the more painful it is to remove.
The nurses will usually clean the area and apply Instillagel before removing the catheter. For me, depending on how much Instillagel is applied and how competent the nurse is, sometimes it can be removed as quickly as a plaster. However, other times it can be a long, drawn-out process with continuous pain.
Of course, if you have paralysis, better muscle control and a stronger pain threshold, changing catheters will be pretty much pain-free
2. Catheters cause infection
This can be true, but can be less frequent and even prevented as long as you look after your catheter. Drinking plenty of water, cleaning the area and flushing the tube can help to prevent urinary tract infections (UTCs).
Medical professionals say indwelling catheters are more prone to infections but luckily, in the four years I’ve had my catheter, I’ve only had infections a couple of times, and that was usually due to self-inflicted dehydration.
Thankfully, since purchasing myself a Hydrant water bottle on the Disability Horizons Shop, I’ve been able to drink on the go and therefore stay hydrated more throughout the day. It has a flexible tube and bite valve, which makes drinking hands-free and independently possible.

It is also important to wash the skin in the area where the catheter enters your body. If this is in your stomach, use mild soap and water, as I do. But if it’s in your urethra, just use water or a product specially designed for intimate areas.
Furthermore, I use sodium chloride 0.9% catheter maintenance solution (salty water) to flush the tube and balloon. This also washes out my bladder to clear out any debris to prevent blockages, keeps the tube and balloon clean and stops future infections. This can be administered independently or by the assistance of a carer.
I flush my catheter once a week, but other people may do it every day, several times a day or just when symptoms of a blockage appear.
3. Catheters worsen incontinence
This is untrue. In fact, it does quite the opposite. If you have a weak bladder and limited to no control of your urine, a catheter can be a huge lifeline.
This is especially the case with an indwelling catheter, which can be attached to a leg bag, meaning you can simply pee to your heart’s content.
There is still the chance of leakages if you have a kink in your tube that is stopping the urine from flowing through. Leakages can also be caused by blockages in the balloon or tube, which is why it is important to flush with a sodium chloride solution frequently.
In addition, incontinence can happen if you have bladder spasms. I experienced this back in 2019. To resolve this I was admitted to the hospital in February 2020 for botox injections in the bladder to essentially relax the muscle wall to stop the spasms. This made all the difference because two and half years on, I do not have any more bladder spasms.
4. Catheters need emptying frequently
Not necessarily. It depends on how much fluids you consume. I tend to empty mine two to three times a day – morning, evening and when using the toilet to open my bowels.
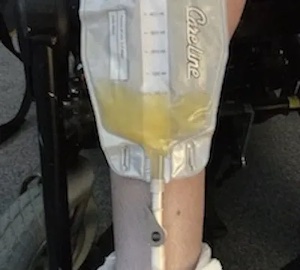
According to the NHS, an indwelling catheter can either drain into a bag attached to your leg, which has a tap at the bottom so it can be emptied (like mine), or it can be emptied into the toilet directly, using a valve.
You should empty the bag before it’s completely full (around half to three-quarters full) and at regular intervals throughout the day to prevent urine from building up in your bladder.
Leg bags and valves should be changed every seven days. The bag can be attached to your right or left leg, depending on which side is most comfortable for you.
I admit, there have been times where I’ve forgotten to empty my urine and my knee looks like it has swelled up or I suddenly have the urge to pee.
On some rare occasions, when I’m alone and have no one to help me empty my bag, it gets so full that I fully soak my clothes and wheelchair. Therefore, as soon as my leg bag looks big or I know I’ll be alone for an hour or more, I empty it again to be on the safe side.
If you have intermittent catheters, timings can vary. For some, as soon as you feel the need to pee, you immediately catheterise. If you have paralysis, you won’t be able to feel the need to go, so it is a case of planning ahead and organising your toilet breaks frequently and roughly at the same times each day.
5. Catheters make using public toilets more difficult
From a practical point of view, definitely not. From society’s perceptions, there can be challenges.
For me, this was one of the reasons I wanted to be fitted with a suprapubic catheter. Accessing public toilets can be a nightmare as a wheelchair user. I require a hoist, toileting chair and changing table to go to the toilet.
I’m aware there are Changing Places toilets, but there aren’t enough of them and sometimes the room is still too small, the toilet is locked or the equipment is not working or broken.
Having a catheter means I can access a standard disabled toilet, empty my urine into a bottle and then empty the bottle into the toilet.
Sometimes, if I can’t find an accessible toilet, I’ll hide in a secluded corner, empty my bag into the bottle then either take the bottle home to empty or send my mum, a PA or friend to the ladies toilets to empty it.
However, if you have hidden impairments or long-term health conditions and catheterise, there can be challenges.
If you use a non-disabled men’s or women’s toilet, you’ll have to catheterise in the toilet cubical and then go back out to clean and dispose of medical supplies, potentially in front of other people using the sinks, hand-dryers and/or urinals, which can feel embarrassing.
Accessible toilets have a sink and clinical waste bin in reach, which will make it a lot easier. But, although you are entitled to use a disabled toilet, some people may judge, assuming that you aren’t disabled because you do not have a visible impairment.
6. Catheters stop you from travelling abroad
Again, this is not true. If anything, it means you don’t have to worry about needing the toilet on long journeys. In some cases, if you empty your bag or self-catheterise before you leave, you may not need to use the toilet again until you reach your destination.
In a car, if the leg bag gets full, you can empty it into a bottle and have it emptied at your next stop or at your destination.
On a train or plane, you can empty the bag into a bottle and either yourself, your companion or a train guard/flight attendant can dispose of it in the train/plane toilets. Or, if you have the ability, you can self-catheterise on the train/plane toilets.
If you are on a longhaul flight and cannot access the plane toilet due to your physical impairment, you could attach your catheter to a night bag, which has a bigger capacity, so that more urine can be collected throughout the journey. You can store the night bag in a handbag or rucksack to disguise it from other passengers. There are some more useful tips for flying with a urinary catheter here.
7. Catheters stop you from having sex
Using a catheter does not stop you from having sex, but some adjustments may be required to accommodate it. If you have an intermittent catheter or a suprapubic catheter, you should be able to have sex as usual.
Indwelling catheters can be more problematic, but it’s still usually possible to have sex with them in place. For example, men can fold the catheter along the base of their penis and cover them both with a condom. Women should be able to tape the catheter up onto the stomach.
You should only use water-based lubricants to assist with sexual intercourse. Other lubricants may damage the catheter.
In some cases, you may be taught how to remove and replace the catheter so sex is easier for you.
8. Catheters are time-consuming
Absolutely not. This is the most vital and valuable reason why I chose to have a catheter.
Before being fitted with my suprapubic catheter, I would have to be hoisted onto the toilet four to five times a day just to pee. This would take 30 minutes each time, taking up to three hours of my day.
Now, with my catheter, I can empty my bladder in two minutes, giving me the rest of the day to work, socialise and relax. I’m sure this is the same for the majority of catheter users.
The only time-consuming part for me is waiting for the district nurses to arrive and prepare for my six-week catheter change.
Check out Emma’s blog series of her future with a suprapubic catheter on her site Rock For Disability.
Do you use a urinary catheter? Can you relate to some of the experiences Emma shared about living with catheters? Or have you learnt more about catheters after reading this article? Share your thoughts with us on Facebook and Twitter @DHorizons.
By Emma Purcell
Image at the top of the article: ©marekuliasz via Canva.com
Additional Tips for Living Comfortably with a Catheter
To enhance your experience with a urinary catheter, consider the following:
- Stay Hydrated: Drinking plenty of water helps prevent infections and keeps urine flowing smoothly.
- Regular Cleaning: Clean the area where the catheter enters your body daily with mild soap and water to reduce the risk of infection.
- Avoid Kinks: Ensure the catheter tube is free from kinks to allow urine to flow easily into the drainage bag.
- Empty the Bag Regularly: Empty your drainage bag before it becomes too full, typically when it’s about half to three-quarters full.
- Monitor for Signs of Infection: Be aware of symptoms like cloudy urine, a strong odor, or discomfort, and contact your healthcare provider if they occur.
For more detailed information on catheter care, visit the NHS guide on living with a urinary catheter.
Catheter Care FAQ
How do I prevent UTIs with a catheter?
Talk to your doctor or nurse who can provide you with detailed instructions on how to properly clean and maintain your catheter, reducing the risk of urinary tract infections. General practices include regular cleansing of the catheter site, maintaining a sterile collection system, and staying well-hydrated.
What are the signs of a UTI?
Signs of a UTI may include persistent urge to urinate, burning sensation while urinating, cloudy or strong-smelling urine, and lower abdominal pain. In severe cases, you may also experience fever, chills or back pain.
How do I change my catheter?
Changing a catheter is usually done by a medical professional to avoid complications or infections. If you are to change it at home, you should first wash your hands thoroughly and work on a clean, flat surface. Use sterilized equipment, follow your provider’s instructions carefully, and always seek medical help if you experience difficulty or discomfort.
How do I care for my catheter site?
To care for your catheter site, clean it daily with warm water and mild soap. Avoid pulling or tugging on the tube. Check regularly for any signs of infection, such as redness, swelling or discharge, and report any issues to your medical provider immediately.
What are the risks of using a catheter?
Potential risks of using a catheter include urinary tract infections, bladder stones, kidney damage, and blood in the urine. Long-term use can sometimes result in reduced bladder muscle tone. Talk to your healthcare provider about any concerns or symptoms.
Additional resources:
UK resources
- NHS urinary catheters: https://www.nhs.uk/conditions/urinary-catheters/
- Royal College of Nursing catheter care guidance: https://www.rcn.org.uk/Professional-Development/publications/catheter-care-guidance-for-health-care-professionals-uk-pub-009-915
- NICE quality statement 4: Urinary catheters: https://www.nice.org.uk/guidance/qs61/chapter/quality-statement-4-urinary-catheters
- NHS urinary catheter tools: https://www.england.nhs.uk/patient-safety/urinary-catheter-tools/
- Shropshire and Telford and Wrekin Local Health Economy E. coli blood stream infection reduction group: https://www.england.nhs.uk/patient-safety/urinary-catheter-tools/
More on Disability Horizons…
- 8 misconceptions about cerebral palsy busted
- 6 misconceptions about ventilators debunked
- All you need to know about the RADAR key scheme to access disabled toilets
- 7 accessible bathroom aids that will give you greater independence and dignity
Originally posted on 31/08/2022 @ 5:54 pm