When Misdiagnosis Leads to Locked-in Syndrome: Understanding Your Options and Support
Locked-in Syndrome (LIS) is a rare neurological condition that can change how someone communicates and interacts with the world. It is often linked to damage in the brainstem, and while the body may be paralysed, awareness and cognition can remain intact. This article looks at what LIS is, how misdiagnosis can sometimes play a role, and the different types of support available—from healthcare and community resources to legal guidance.
Key facts about Locked-in Syndrome and support options
| Topic | Key point |
|---|---|
| Locked-in Syndrome | Paralysis with preserved awareness, often affecting movement and speech |
| Communication | Eye movement, blinking, and assistive technology enable interaction |
| Misdiagnosis risks | Delays in treatment can affect outcomes in some cases |
| Daily life | Relies on accessible environments, support networks, and adaptive tools |
| Support options | Healthcare, charities, peer networks, and practical adaptations |
| Legal considerations | One possible route when care standards may not have been met |
What is Locked-in Syndrome?
Locked-in Syndrome is usually caused by damage to the brainstem, often following a stroke. A person may lose voluntary muscle movement, including speech, while remaining fully aware of their surroundings. Many people with LIS can still move their eyes or blink, which becomes an essential way to communicate. A peer-reviewed first-person account published in the BMJ, titled The patient’s journey: Living with locked-in syndrome, offers rare insight into what this preserved awareness actually feels like from the inside.
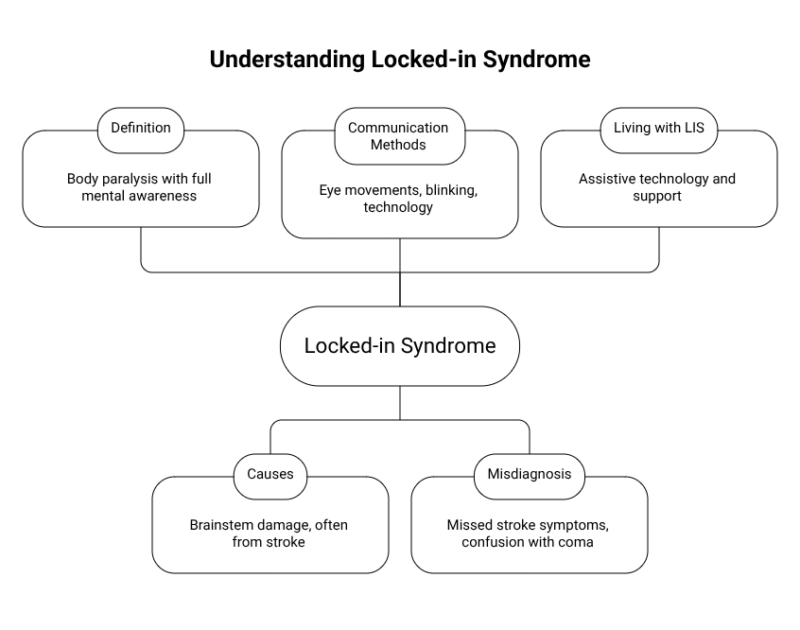
Communication methods vary. Some people use eye-tracking technology or alphabet boards, while others rely on subtle facial movements. Experiences differ widely depending on the extent of neurological damage and the support available.
How misdiagnosis can contribute
In some situations, delays or errors in diagnosis may affect how quickly treatment begins. This does not always lead to LIS, but timing can be critical in neurological conditions. In one documented UK case, Lisa — a mother-of-two from Bishops Stortford — was sent home from Addenbrooke’s Hospital in 2016 after presenting with left-side
paralysis, told her symptoms may be stress-related. She suffered a second stroke overnight. Cambridge University Hospitals NHS Trust later admitted a breach of duty of care, and Lisa
was awarded £1 million in compensation. Her solicitor described it as “an utterly preventable situation.”
- Delayed recognition of stroke symptoms
- Infections that are not identified or treated promptly
- Medication or electrolyte imbalances
- Missed underlying risk factors, such as clotting disorders
These situations are often complex. Outcomes depend on many factors, including how quickly care is provided and how the body responds.
Living with Locked-in Syndrome: daily realities
Life with LIS is shaped not only by the condition itself but by the environment around the person. Barriers such as inaccessible communication tools or limited support can make daily life more difficult.
Assistive technology plays a central role. Eye-tracking devices, speech-generating software, and adapted computers allow people to communicate, work, and stay connected. Access to these tools can vary, which highlights the importance of inclusive design and funding support.
Carers, family members, and support workers are often key to day-to-day life.
Their role goes beyond physical assistance—they help interpret communication, support decision-making, and maintain social connections.
Emotional adjustment can also be part of the experience. For example, someone who previously communicated verbally may need time to adapt to using assistive technology. With the right support, many people continue to take part in conversations, relationships, and creative work.
Real experiences of Locked-in Syndrome
Behind the clinical descriptions are real people navigating extraordinary circumstances. Kate Adamson had a stroke at 33, was left with Locked-in Syndrome, and given a grim prognosis. She went on to recover and became a disability advocate and hospital social worker — her story is documented by the American Heart Association and is one of the better-known accounts of long-term recovery from LIS.
In online communities, people who have lived through LIS describe just how fine the line between diagnosis and misdiagnosis can be.
One person who shared their experience publicly described being incorrectly assessed as brain dead while fully conscious throughout — their only means of signalling awareness was an almost imperceptible tongue movement. Their account underlines why awareness of LIS matters in clinical settings.
Support beyond medical treatment
Support for people with LIS extends well beyond hospital care. A combination of services and community connections can make a meaningful difference.
- The Brain Charity
— the UK’s only charity covering all 600+ neurological conditions — offers
counselling, befriending, and a dedicated Locked-in Awareness programme - The Stroke Association provides guidance and peer support for stroke survivors
and their families - Rehabilitation services through the NHS may include physiotherapy, speech and
language therapy, and assistive technology assessments - Peer networks connect people with shared experiences, reducing isolation
- Accessible housing and community environments help remove everyday barriers
Some people also explore practical tools that support independence, such as
assistive tools for daily living, which can help create more accessible routines at home or in work settings.
When a medical error may be a factor
In some cases, people may question whether earlier diagnosis or different treatment could have changed the outcome. It is not always possible to determine this clearly, and medical situations are rarely straightforward.
Research into brainstem strokes has found that LIS is sometimes initially mistaken for coma or vegetative state, partly because standard neurological assessments can miss preserved awareness if eye movement is not specifically tested.
The Brain Charity notes that early and accurate diagnosis is critical to beginning appropriate communication support.
Raising concerns can be part of understanding what happened. This might involve reviewing medical records, asking questions, or seeking independent advice.
Understanding your legal options
For some families, exploring legal advice is one way to understand whether standards of care were met. This process usually involves reviewing evidence, timelines, and medical decisions. Cases like Lisa’s — where an NHS Trust admitted a breach of duty following a missed stroke diagnosis — show that pursuing a claim can be a legitimate route for some families.
If you’re trying to understand whether a delayed diagnosis played a role, speaking with a Locked-in Syndrome lawyer can help clarify what evidence is needed and whether pursuing a claim is appropriate.
For USA readers, speaking with a Locked-in Syndrome attorney is a good starting point.
In the UK, the NHS Resolution process or a solicitor specialising in clinical negligence — many of whom offer free initial consultations under a no win, no fee arrangement — is typically the first step for families considering a claim.
Legal action is not the right choice for everyone. Some people focus on rehabilitation, ongoing care, or advocacy work instead. Each situation is personal, and there is no single path to follow.
Financial and practical considerations
Living with LIS can involve long-term planning. This may include:
- The cost of care and support workers
- Specialist communication equipment
- Home adaptations for accessibility
- Transport and mobility arrangements
Funding can come from a range of sources, including NHS support, local authority services, or personal funding. Access often depends on local systems and eligibility criteria.
Final thoughts
Locked-in Syndrome changes how someone interacts with the world, but it does not remove their ability to think, communicate, or take part in life. With the right support, many people continue to express their views, maintain relationships, and shape their own decisions.
Support looks different for each person. It may involve healthcare, community networks, practical tools, or legal advice. What matters most is having options and access to the support that fits individual needs.